
Medical ethics is described as the moral construct focused on medical issues affecting patients and medical practitioners. It is a field that formally considers the morality or potential problems of medical decision-making and used as the basic principles in developing the code of ethics in healthcare providers, as first depicted in the Hippocratic oath. The principal objectives in the medical profession are to render service to humanity with full respect for the dignity of profession and man.
In light of the COVID-19 pandemic, the framework of healthcare has shifted from a patient-first-dominant framework to a public-health focus. The basic principles of bioethics are still the same, but the application will be applied for not only individuals. The goal of patient care should remain the same; to strive for the best clinical outcomes while minimizing harm and risk of disease transmission. The principle of non-maleficence should remain applied.

The implementation of medical ethics faces crises during the COVID-19 pandemic. With limited resources and a massive influx of patients, the theoretical risk of sacrificing the most vulnerable patients has shaken the ethical beliefs. For example, a triage plan with ethical justifications for ICU has been proposed to maximize the benefit for the greatest number of people.
- Prioritize those most likely to survive the current illness
- Prioritize those most likely to live the longest after recovery, considering comorbid conditions
- Prioritize those who have lived fewer life stages
- Prioritize those who have a narrow social utility to others in a pandemic
Among the ethical principles considered, prediction of lifespan is used as the priority selection criterion, which means that the youngest individuals should receive priority. However, this principle of doing the greatest good for the greatest number may be inadequate as it ignores other ethically relevant considerations.
Other than in clinical settings, ethical dilemmas also happen in society.
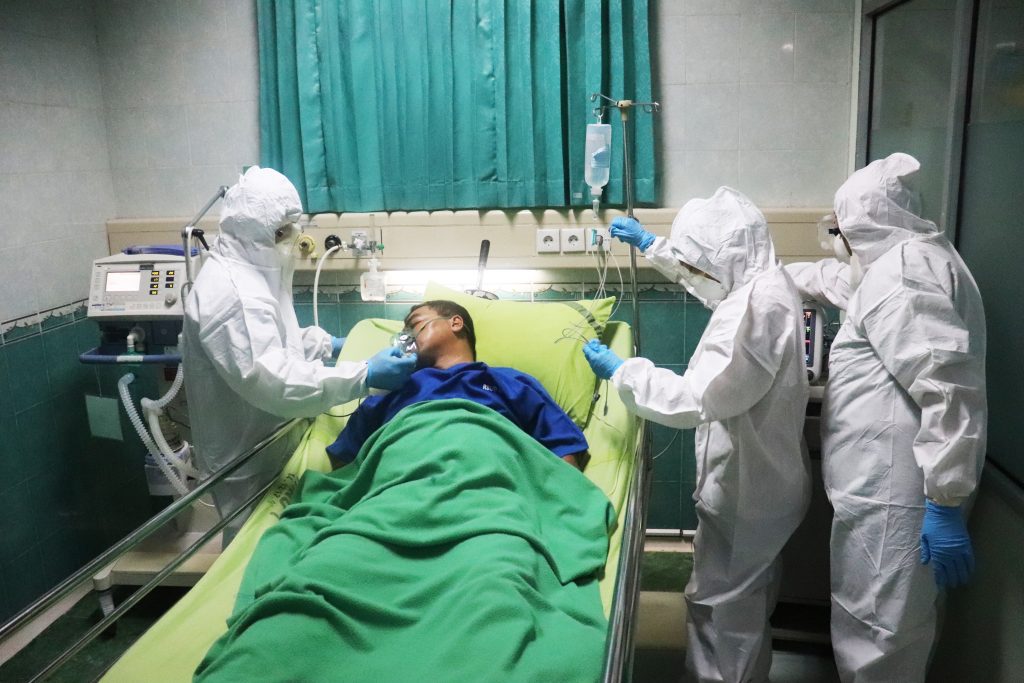
To ensure preventive care, is it acceptable to publicly disclose information about COVID-19 patients?
“Where has the patient been?” and “Who is the patient?” were the questions that arise when cases of COVID-19 patients are announced. Contact tracing is important when an infectious disease is identified in a community, yet it is a part of the patient’s privacy. In this digital era, the act of ostracizing a person becomes a habit. With this situation, people are more anxious to get tested for SARS-CoV-2 because they’re worried that their name will be publicly announced and get shunned by their neighbors. Nevertheless, as learned over the years, handling an infectious disease can be just as effective without mentioning names. As stated on Pasal 51 Undang-Undang Nomor 29 Tahun 2004, a doctor has the obligation to keep the patient’s information confidential. Yes, contact tracing is important to alert the relevant public, but to decide whether naming names are required or not needs further considerations.

For healthcare workers who are putting themselves at risk for COVID-19 patients, what are the ethical obligations of society for them?
The healthcare institutions or employers are obliged to make sure that there is a sufficient amount of protective equipment, masks, filtered air, and other materials that allow them to work in a safe environment. Doctors and nurses take professional oaths that they will respond in the time of emergency. Meanwhile, the janitors, the people who clean the rooms, and the people who are in charge of food service in hospitals never took that oath. It is important that we are also mindful of protecting them; making sure that they allocated a safe working condition and allow them to opt out if they don’t feel safe when sufficient protections can’t be provided.
As the threat of COVID-19 continues to rise in developing countries especially in Indonesia, it is our duty as youths and medical students to maintain the trust between patients and communities and guard our healthcare workers against moral distress or burnout. Some of the ethical principles that we, as medical students, can apply in our daily life are about advocacy and empowerment, also about providing information. As the usage of social media has increased significantly during these times, it is one of our obligations to inform, educate, and empower people about health issues. It is important that false and misleading information are being tackled. Hence, we begin to correct the gaping health disparities that currently exist. Without doing so, we cannot truly be rid of COVID-19.
REFERENCES:
Chew, C. and Ko, D., 2020. Medical ethics in the era of COVID ‐19: Now and the future. Respirology, 25(10), pp.1033-1034.
Emanuel EJ, Persad G, Upshur R, Thome B, Parker M, Glickman A, et al. Fair allocation of scarce medical resources in the time of Covid-19. N Engl J Med. 2020;382:2049–55.
Farlex Partner Medical Dictionary. (2012)
Maves RC, Downar J, Dichter JR, Hick JL, Devereaux A, Geiling JA, et al. Triage of scarce critical care resources in COVID-19 an implementation guide for regional allocation. Chest. 2020. https ://doi.org/10.1016/j.chest.2020.03.063.
Robert, R., Kentish-Barnes, N., Boyer, A., Laurent, A., Azoulay, E. and Reignier, J., 2020. Ethical dilemmas due to the Covid-19 pandemic. Annals of Intensive Care, 10(1).
Undang-Undang Republik Indonesia Nomor 29 Tahun 2004 tentang Praktik Kedokteran
Vergano M, Bertolini G, Giannini A, Gristina GR, Livigni S, Mistraletti G, Riccioni L, Petrini F. Clinical ethics recommendations for the allocation of intensive care treatments in exceptional, resource-limited circumstances: the Italian perspective during the COVID-19 epidemic. Crit. Care 2020; 165: 1–3.
White, P., Cohn, R. and Humbyrd, C., 2020. Medical Ethics During A Public Health Crisis.



